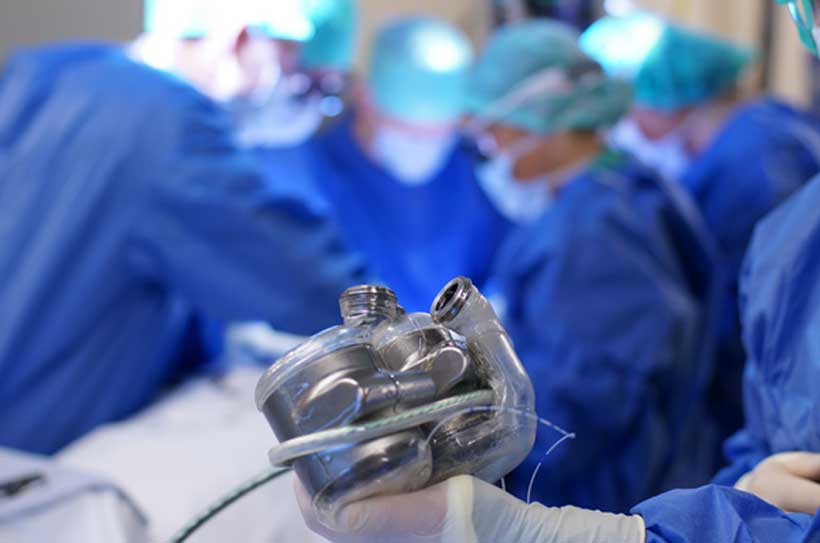
The human heart beats 100 000 times a day, every beat circulating blood, oxygen and nutrients to all parts of the body. Heart failure happens when the fist-sized organ is unable to perform this vital function properly.
Most people with the condition are forced to seek long-term mechanical support for blood circulation. While pumps and artificial hearts have been available for more than 40 years, the options currently on offer are tricky for their users.
New normal
The devices are often noisy and require patients to carry heavy battery packs and have wires going through their skin to power the device. Some even use pumps outside the body to circulate the blood.
But researchers are hopeful that a new generation of artificial hearts will improve things.
‘Our vision is that one should be able to live a completely normal life with an artificial heart,’ said Ina Laura Perkins, co-ordinator of the EU-funded ArtOfHeart project.
Heart failure dramatically affects quality of life. Normal activities such as taking the stairs, engaging in domestic chores or even putting on clothes become difficult.
It also makes participating in social activities and keeping a job challenging. Once patients have reached the point of severe heart failure, they are often bedridden.
Cardiovascular disease kills 3.9 million people in Europe every year, accounting for 45% of all deaths. The European Heart Network estimates that more than 10 million people in the EU are likely to be affected by heart failure.
While transplants can offer a solution, only a select few patients are added to waiting lists for such an operation as a result of a severe worldwide shortage of donor hearts. Consequently, the prospect of an effective artificial alternative offers a lifeline for many.
As well as being difficult to live with, today’s artificial hearts can also damage the blood.
‘What I think is preventing artificial hearts from really realising their full potential is the blood-related complications that patients suffer,’ said Perkins.
Swedish tests
ArtOfHeart, partly funded by the European Innovation Council (EIC), is investing €38 million to conduct clinical and pre-clinical testing of an artificial heart developed by Swedish company Scandinavian Real Heart AB.
The problem with current devices, according to Perkins, is that the mechanical flow they generate can create a lot of stress on the blood, damaging and deforming cells. This in turn can lead to clotting, thrombosis and strokes.
For instance, some artificial hearts circulate the blood using a propeller-like device rather than a pump. This creates a continuous blood flow instead of a pulse and causes a lot of force at the blade edges.
The artificial heart being tested claims to be the first designed to closely mimic the structure of the human heart. It consists of two pumps that each have an atrium, a ventricle and a pair of mechanical valves. The idea is that the more natural blood flow produced in this way will reduce the complications that can arise with existing devices.
To gain regulatory approval, Real Heart is exploring its device’s reliability and impact on blood in a series of laboratory tests. The company is also conducting a series of animal studies in sheep. The team aims to begin clinical trials in around 10 patients in 2024 and have the artificial heart on the market in 2026.
The first version will be connected by a cable through the skin to a battery belt. The hope, however, is that in the future this cable connection will not be needed.
‘Our device is very energy-efficient, so it opens up the possibility of doing wireless charging through the skin,’ said Perkins.
With such a setup, patients would wear a vest or a belt around their chest to provide the wireless charge. In the meantime, the device’s energy efficiency means that the battery packs patients have to carry should be relatively small and light compared with other artificial hearts.
Inflatable balloons
Another EU project is developing an artificial heart using soft robotics. Funded by the EIC’s Pathfinder programme, HybridHeart is seeking to create artificial muscles that mimic the contraction of the heart’s natural muscles.
The resulting artificial heart can be thought of as a set of complex balloons, according to Bas Overvelde, an expert in soft robotics at Eindhoven University of Technology in the Netherlands and a member of the multidisciplinary HybridHeart team.
The device has an internal chamber that holds the blood. When the balloons are inflated, the internal chamber contracts and pumps the blood around the body.
‘Instead of having a heart muscle, like in our natural heart, we have these soft actuators that cause contraction of the heart,’ Overvelde said.
Pumping the blood in this way spreads the force and the stresses across the whole chamber, just like in a human heart, he said. This enables a gentler motion and should reduce localised stresses that can damage blood cells.
More freedom
While the basic workings of the device may seem simple, getting it to work well is complex, according to Overvelde.
For instance, as a result of their structure, the stiffness of a heart’s tissues changes in response to alterations in blood pressure. This leads to an automatic adjustment in the heart’s pumping force and rate.
The hope is that the soft robotics can provide the HybridHeart device with a similar feedback mechanism to regulate its beating.
To provide patients with more freedom and a better quality of life, Overvelde said that energy efficiency is key.
‘At the moment, we are aiming for the device to be wirelessly charged, and for a half hour to an hour untethered, so that you can take a shower,’ Overvelde said. ‘It is essential that you can be untethered for a little while, so that you can temporarily be disconnected from any external battery.’
The HybridHeart project is testing the artificial heart in goats and sheep. The hope is to progress to clinical trials in around seven years, a step that will require additional funding.
While the device probably won’t be better than a natural-heart transplant, Overvelde says there are too limited a number of those available for all the patients in need of such an operation.
Perkins echoes this view, stressing that patients are dying because of a lack of transplants and good alternatives. This is the void artificial hearts need to fill.
Research in this article was funded by the EU. If you liked this article, please consider sharing it on social media.
Research in this article was funded by the EU. This article was originally published in Horizon, the EU Research and Innovation Magazine.